“Riot Sweeps Chicago” should sound and feel intuitively familiar. However, this headline covered the front pages of a newspaper over a hundred years ago. Named the “Red Summer of 1919”, a spate of violence and bloodshed occurred from April to November 1919 with riots, lynchings, and mobs across the country. Hundreds of African American lives were claimed and hundreds more were left maimed and homeless. The most violent episodes occurred in Chicago, IL, Washington, D.C. and Elaine, AR and were precursors for what many are now learning to be the Black Wall Street Massacre in Tulsa.
Signifying the Red Summer, Eugene Williams, an African American teenager, violated the unofficial segregation of a Chicago beach and then was stoned by a man, who was part of a white mob, and then subsequently drowned. The terrorizing racism that followed ignited one of the longest and bloodiest race riots ever witnessed in the country. Similar to today, these racist incidents that captured national and international attention came on the heels of a pandemic—the 1918 influenza outbreak.
Fast forwarding to a century later, the COVID-19 pandemic, the murder of George Floyd and the protests demonstrations attended by millions, as well as the insurrection of 2021, all mirror a place that we have seen before in this country. It seems that syndemics, or rather the aggregation of multiple epidemics (e.g., coronavirus, police brutality), followed by racial violence are the strands that make up America’s DNA.
During the COVID-19 pandemic, the murder of George Floyd ignited global attention to police brutality and systemic racism in the United States. In spite of social distancing recommendations, mask wearing Black Lives Matter protesters flooded the streets across the world during a “Racial Reckoning Summer of 2020.” From late May until the end of June 2020, roughly 20 million people in the United States participated in demonstrations over the death of George Floyd, as well as Breonna Taylor, another Black body, among many, perceived to be discriminatorily targeted and killed by police.
Following the murder of George Floyd, systemic racism was finally classified by many as a public health crisis. This was for good reason. Structural racism also fortifies and informs policies in the United States that perpetuate racial disparities in health outcomes, inequalities in health determinants, such as housing, education and healthcare, as well as through the discriminatory policing of African Americans. Beyond the mortality of police violence, research has shown that this type of violence also contributes to negative health outcomes, such as psychological stress leading to stroke or accelerated aging.
In order to fundamentally address the race based health disparities of COVID-19 and so many other conditions that disproportionally worsen the health of African Americans, we have to move beyond the person-centered approach and stop pushing policies that “blame” the sick and “reward” the healthy. Health policies need to, now more than ever, reflect the role of social determinants, or rather the conditions (e.g., health care access; affordable housing; employment) that influence and shape disease risks for individuals and populations, as well as, the structural racism that saturates the policies of these determinants. Once the magnitude of these determinants are fully appreciated, health policy strategies and solutions imbued with an ecological model that aims to understand the multiple and interacting determinants of health behaviors at many levels [(interpersonal (e.g., family), organizational (e.g., workplace), community (e.g., neighborhood), public policy (e.g., state laws)] beyond the individual can then begin to tackle the health inequity issues that were present long before the COVID-19 pandemic began.
But, social change must expand beyond health care. To transform and reorient this country into an antiracist society, or one that ensures equity and justice for all by consciously fighting against racism on individual and institutional levels, the question, from Dr. Ibram X. Kendi, “what is wrong with policies?” needs to be asked and followed with action. From corporate America and small businesses to institutions and not-for-profits, leaders and stakeholders at all levels should aim to address the following:
- Confront racist ideologies, including one’s own, with the utmost level of intolerance
- Create programs, measures, and systems of accountability for antiracist policies
- Develop a systematic approach to assessing and monitoring the cultural climate
- Promote education and dialogue about racism, its causes, and effects
- Apply intersectionality to understanding interdependent systems of discrimination
- Commit to identifying and dismantling racial inequities and disparities
- Leverage your position of power to champion antiracist practices and policies
Today, many people think that pandemics and protests have never uniquely come together in this country, but they would be wrong. We have been here before. The question is what will happen now to prevent history from repeating itself in the decades ahead. In order for this moment to not just be a fleeting one that recognizes the impacts of historical and contemporary racism and does little to change policies, the recommendations above should strongly be considered to achieve an antiracist society and repair the damage of racial discrimination.
Jennifer D. Roberts is an Assistant Professor in the Department of Kinesiology, School of Public Health at the University of Maryland College Park (UMD) and Founder and Director of the Public Health Outcomes and Effects of the Built Environment (PHOEBE) Laboratory. Her scholarship focuses on the impact of built, social, and natural environments, including the institutional and structural inequities of these environments, on the public health outcomes of marginalized communities.
The Brookings Institution is committed to quality, independence, and impact.
We are supported by a diverse array of funders. In line with our values and policies, each Brookings publication represents the sole views of its author(s).


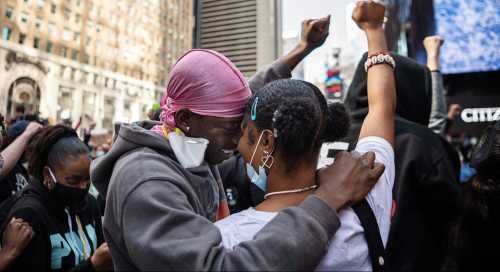




Commentary
Pandemics and protests: America has experienced racism like this before
June 9, 2021