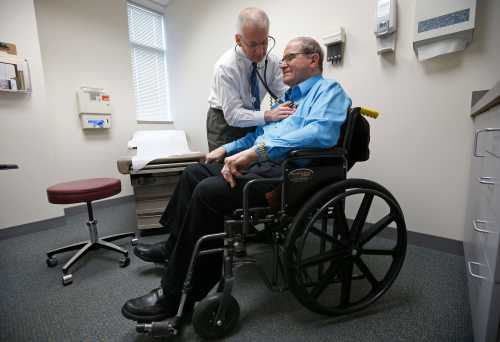
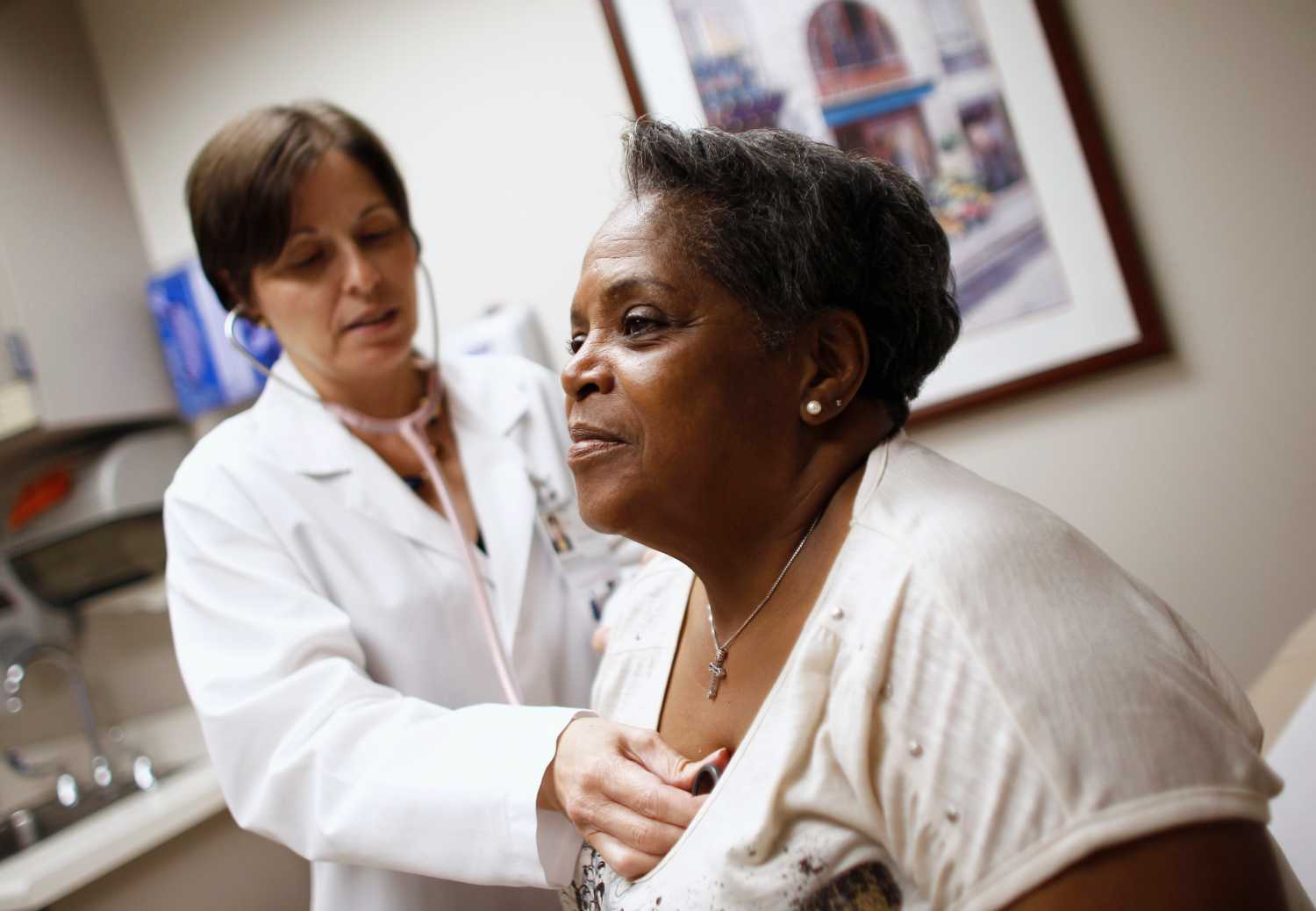The Affordable Care Act (ACA) changed the nature of competition among health plans by creating regulated insurance exchanges, introducing new insurance industry regulations, and providing premium and cost-sharing reduction subsidies. Through these reforms, the law aimed to increase access to and the value of insurance coverage while lowering costs. To better understand the law’s implementation and its effect on competition, researchers with the ACA Implementation Research Network interviewed key marketplace stakeholders to analyze why carriers chose to enter or exit markets, how provider networks were built, and how state regulatory decisions affected the landscape.
As Congress and the new Administration deliberate on what’s next for the law, the Network presents their analyses of competition in California, Florida, Michigan, North Carolina, and Texas (PDFs). A summary report (PDF) of the general findings, authored by Texas A&M Professor Michael Morrisey, Brookings Senior Fellow Alice Rivlin, ACA Network Lead Richard P. Nathan, and Mark A. Hall, Brookings Nonresident Senior Fellow, is intended to generate hypotheses for further testing across state marketplaces and to identify individual idiosyncrasies within the states that provide context for national- and state-level reforms.
STATE HIGHLIGHTS
- In California (PDF), Micah Weinberg and Patrick Kallerman of the Bay Area Council Economic Institute report that the state’s uninsured population was cut in half between 2014 and 2017, and many stakeholders attributed this to both the state’s active purchasing model—including aggressively negotiating with insurers over premiums— and their active navigator program—which succeeded in increasing enrollments for individuals between 100 and 200 percent of the federal poverty level.
- In Florida (PDF), Patricia Born of Florida State University noted that respondents in the state see the marketplace as being largely successful, particularly in population-dense areas, and highlighted the positive impact navigators and other consumer-assistance efforts appear to have had in many parts of the state, despite legislation making navigator licensure more difficult.
- In North Carolina (PDF), the participation of Aetna and UnitedHealthcare provided a strong start for the state marketplace. However, Mark A. Hall and Katherine Booth of Wake Forest University report that both insurers withdrew due to higher-than-expected claim costs and the state’s lack of Medicaid expansion. Additionally, the decision of the federal government to refuse to permit a merger between Aetna and Humana likely contributed to Aetna’s decision to pull out, leaving Blue Cross as the dominant insurer in the state.
- In Michigan (PDF), Megan Foster Friedman, Josh Fangmeier, Nancy Baum and Marianne Udow-Phillips at the Center for Healthcare Research & Transformation report that the success of regional insurers over national insurers, particularly Medicaid managed care organizations, is believed to have contributed to the general success of competition in Michigan compared to other states.
- In Texas (PDF), Michael Morrisey and Tiffany Radcliff of Texas A&M University found that the marketplace “unraveled rather dramatically,” when insurers left the marketplace due to higher-than-expected claims and losses from poor risk adjustment procedures, leaving even major urban areas like Houston with only three insurers.
CONCLUSION
While the results of this five-state study may not be applicable across the country, the authors emphasize a few key lessons for further consideration when crafting a potential replacement plan or changes to the law:
- Health insurance markets are local and depend on the ability of insurers to create competitively priced plans. While this is often more difficult in rural locations, metropolitan areas also see variation in competition.
- Higher-than-expected claims costs caused concern for insurers initially, as they lacked information on the amount of health care service utilization to expect from exchange enrollees. It remains to be seen whether the trend will continue or if recent market adjustments reflect a “one-time correction.”
- Insurer networks have narrowed, which potentially provides greater opportunity for insurers to negotiate lower prices by assuring a greater volume of patients to a more limited number of providers. The number of preferred provider organization (PPO) exchange plans has also been decreasing, as these plans had disproportionate enrollment of people with pre-existing conditions and are generally less able to negotiate low prices from providers.
- Both hospital and provider competition are vital for competitive markets, with population and the number of physician groups and health systems playing a role in cost competition.
The Brookings Institution is committed to quality, independence, and impact.
We are supported by a diverse array of funders. In line with our values and policies, each Brookings publication represents the sole views of its author(s).