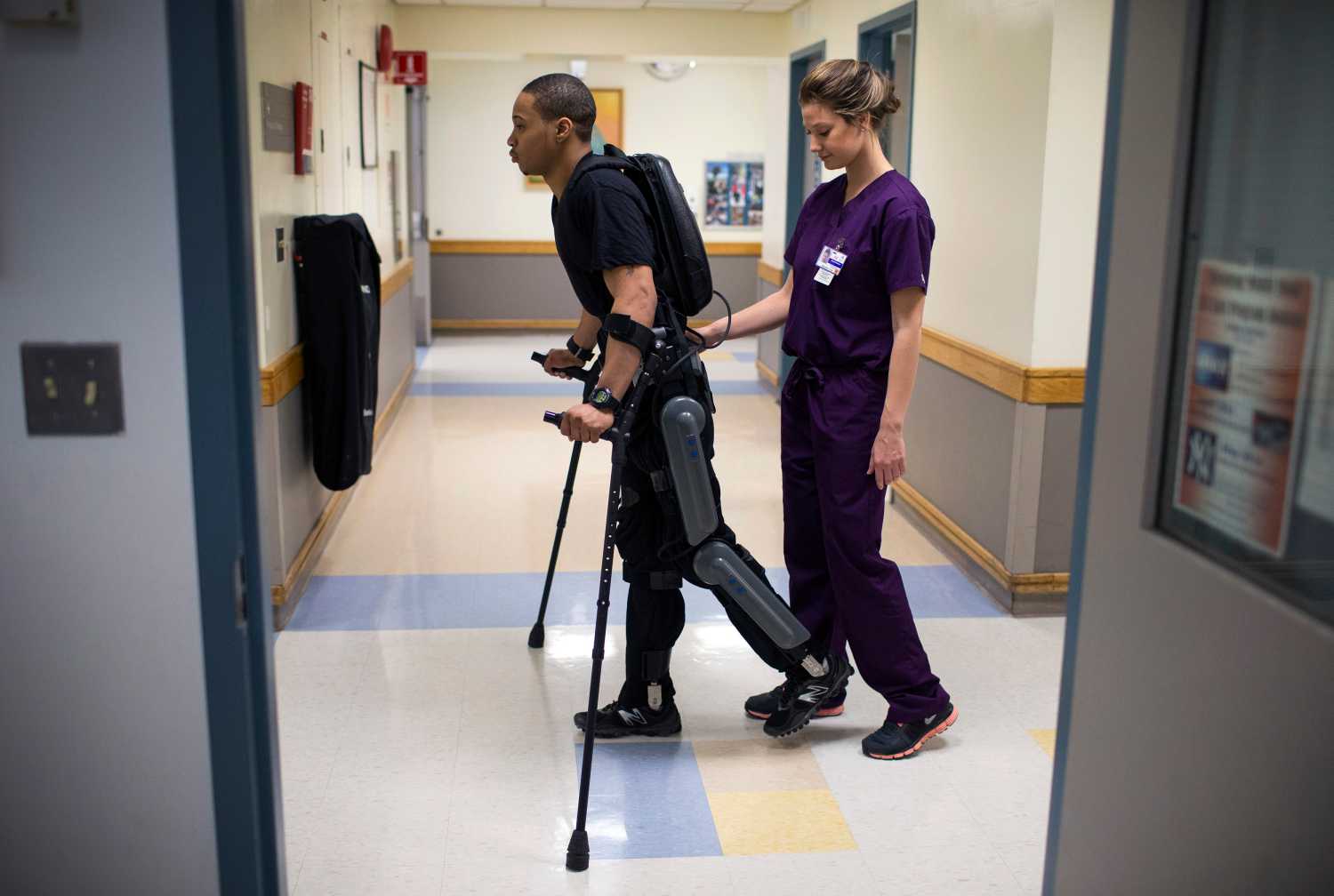
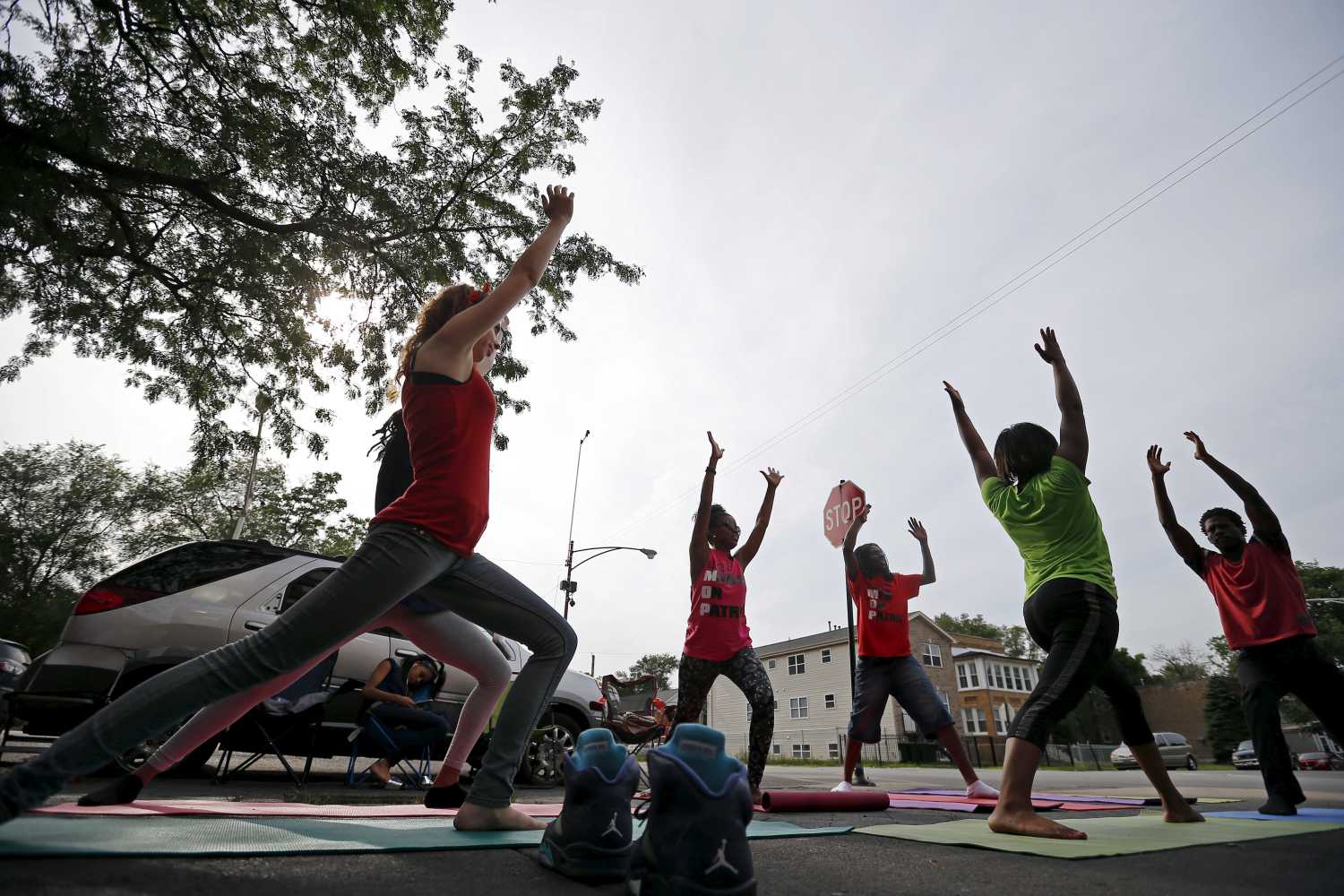In the American health care system, the operations of health facilities often are disconnected from the behavioral and economic drivers in communities that are most related to good long-term health, such as education and housing. This siloed nature of the system contributes to many avoidable readmissions, medical errors, and other adverse patient outcomes.
Intermediaries can bridge this divide by providing key skills and building trust between health care institutions and community organizations and residents. With roughly 3 million professionals in the field, nurses are the largest segment of the US health care workforce and have enormous potential to serve as intermediaries.
In “Nurses as intermediaries in the promotion of community health: Exploring their roles and challenges” (PDF), Stuart Butler and Carmen Diaz review the roles of a variety of nurse specialties. They find that not only do nurses provide skilled health care services, but tend to be the closest to the patient and their family caregivers, and the most aware of their broader psychosocial and health care needs.
But, there are a number of barriers that need to be addressed if nurses are to reach their full potential as intermediaries between patients, the health system, and community institutions. These obstacles include:
- Data silos can make it difficult for nurses to gain access to the information they need. These barriers need to be addressed.
- Scope-of-practice rules and other professional barriers prevent nurses from maximizing their effectiveness. States need to review such rules, and training needs to be appropriately designed.
- Budgets and payment systems often frustrate efforts to use nurses strategically. These need to be aligned to encourage the more effective use of nurses as intermediaries.
The authors conclude that while the understanding of the connection between social conditions and health is growing more needs to be done to make greater use of intermediaries who can can work more directly and consistently with individuals and who have the flexibility and connections to link individuals with medical and other services.
“As we point out in this report, nurses have enormous potential to function as key intermediaries; many are doing so already, and the training and responsibilities of nursing specialties increasingly recognizes this role. But much more needs to be done to empower nurses as intermediaries by addressing data concerns, strengthening the training and professional roles of nurses, and aligning budget strategies.”
Read the full report here.
The authors did not receive financial support from any firm or person for this article or from any firm or person with a financial or political interest in this article. They are currently not an officer, director, or board member of any organization with an interest in this article.
The Brookings Institution is committed to quality, independence, and impact.
We are supported by a diverse array of funders. In line with our values and policies, each Brookings publication represents the sole views of its author(s).