What’s the latest in health policy research? The Essential Scan, produced by the Schaeffer Initiative for Innovation in Health Policy, aims to help keep you informed on the latest research and what it means for policymakers. If you’d like to receive the biweekly Essential Scan by email, you can sign up here.
Private Medicare Advantage plans achieve better outcomes at lower costs for post-acute care than Medicare FFS
“This is a very important look into the “black box” of Medicare Advantage, showing important changes in patient care and outcomes.”
– Paul Ginsburg, PhD, Director of the Schaeffer Initiative
Peter J. Huckfeldt, Jose J. Escarce, Brendan Rabideau, Pinar Karaca-Mandic, and Neeraj Sood find that Medicare Advantage (MA) enrollees receive less intense postacute care and experience better outcomes than Medicare Fee for Service (FFS) beneficiaries during care for lower extremity joint replacement, stroke, and heart failure. Averaged across the three conditions, the authors estimate that FFS costs would be reduced 16 percent per episode if the levels of postacute care provided by MA were carried over to FFS. In the case of joint replacement, only 3.7 percent of MA patients were admitted to inpatient rehabilitation facilities, compared to 11.0 percent of FFS patients, while MA patients were 0.8 percentages points less likely than FFS patients to be readmitted to the hospital within 90 days post-discharge. These findings help explain how MA plans are able to achieve lower costs than FFS and lend evidence to the potential of “bundled payments” to lower costs in FFS without adversely impacting quality of care. Full article here.
Bundled payments for joint replacement reduced spending by 20.8% per episode
Amol S. Navathe, Andrea B. Troxel, Joshua M. Liao and coauthors find that bundled payments for joint replacement saw a decrease in total spending of $5,577, or 20.8 percent, per episode of care without complications. Among those with complications, costs declined $5,321, or 13.8 percent, per episode. A majority of savings were derived from declines in implant prices and high-cost postacute care setting costs; however, postacute care savings were observed only when bundles included financial responsibility for postacute care costs. In addition to overall savings, these findings are encouraging to bundled payment advocates because they highlight the significant impact that changes requiring little-to-no investment, like implant costs and spending associated with high-cost postacute care settings, can have in reducing costs. Full article here.
In-home assessments increased doctor visits for newly diagnosed conditions, yet patients without established provider less likely to seek care
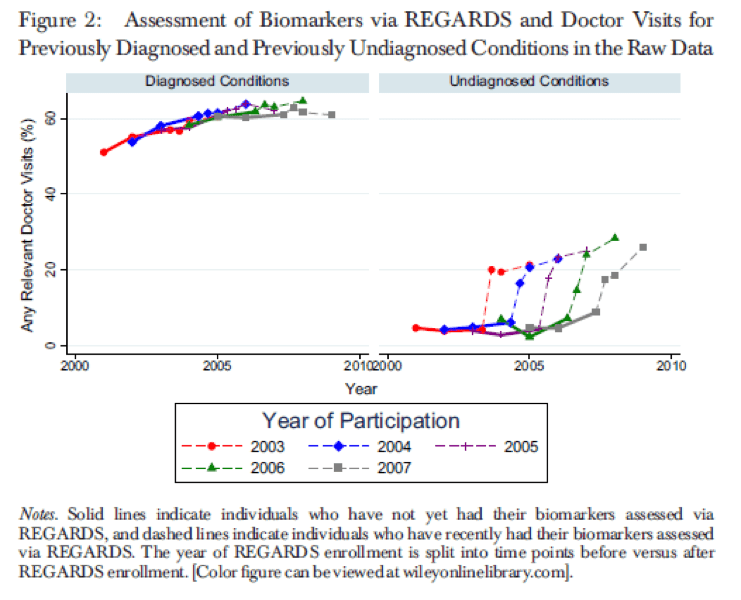
Rebecca M. Myerson, Lisandro D. Colantonio, Monika M. Safford, and Elbert S. Huang find that in-home assessments for high cholesterol, hypertension, and diabetes among previously undiagnosed Medicare beneficiaries spurred a 22 percentage point increase in regular doctor visits for care, with the biggest increase for those found to have diabetes. The authors found no significant differences in care-seeking behavior among those newly diagnosed by gender, race, Medicaid eligibility, income, marital status, or living in a Health Provider Shortage Area; yet, patients without established providers were less likely to visit the doctor for care. Beneficiaries with undiagnosed illnesses at the point of assessment were more likely to both lack a routine provider and have higher blood pressure, fasting blood glucose, total and LDL cholesterol, and lower HDL cholesterol than those previously diagnosed. These findings highlight the impact in-home assessments can have on care-seeking behaviors, as well as underscore the need for new ways to engage hard-to-reach beneficiaries. Full article here.
Innovative medical devices under review 34% longer than subsequent entrants
Ariel Dora Stern finds that innovative medical technologies are under regulatory review for 7.2 months longer—or 34 percent—than subsequent devices, adding an estimated 7 percent to devices’ total cost to bring to market. This finding stands in contrast to the new-entrant advantages seen by breakthrough drugs, which have been found to undergo faster regulatory approval than subsequent drugs. Related to the higher relative development costs, the author finds that small companies are less likely to develop innovative devices than they are innovative drugs. Stern finds that publishing objective regulatory guidelines ameliorates device approval delays. These findings underscore the unique issues facing medical device regulatory review, and may bode well for continued efforts to improve guidelines and transparency of the review process, like the joint Federal Trade Commission and Food and Drug Administration’s 2016 launch of an interactive online tool to support medical device developers. Full article here.
The Essential Scan is produced by the Schaeffer Initiative for Innovation in Health Policy, a collaboration between the Center for Health Policy at the Brookings Institution and the USC Schaeffer Center for Health Policy & Economics.






Commentary
The essential scan: Top findings in health policy research
January 12, 2017