Although the international pharmaceutical industry developed two COVID-19 vaccines in record time, distribution has been frustratingly slow and has revealed serious breaks in the manufacturer-to-patient supply chain.
While the U.S. employed every possible resource to develop the vaccines, we are neglecting to use the best available information technologies to efficiently distribute them. We could do a much better job fighting this pandemical war with weapons we already have.
The most notable example of such powerful-yet-neglected tools are Health Information Exchange (HIE) platforms. HIEs electronically retrieve, organize, and share medical data between clinical points of service, like doctors, hospitals, and specialty care providers (including mental health and telemedicine). While they are designed to exchange lab results, prescriptions, and so-called admission, discharge and transfer records confidentially and securely, they could also be used by public health officials to monitor outbreaks and, importantly, vaccination status.
We used data on COVID-19 vaccinations reported by NBC News to rank the states based on their vaccination rates. As of January 26, 2021, the median vaccination rate is 5,492 per 100,000 residents. Alaska and West Virginia are leading with vaccination rates that are more than two and a half times greater than those of Missouri and Idaho at the very bottom.
COVID-19 vaccination doses per 100,000 population
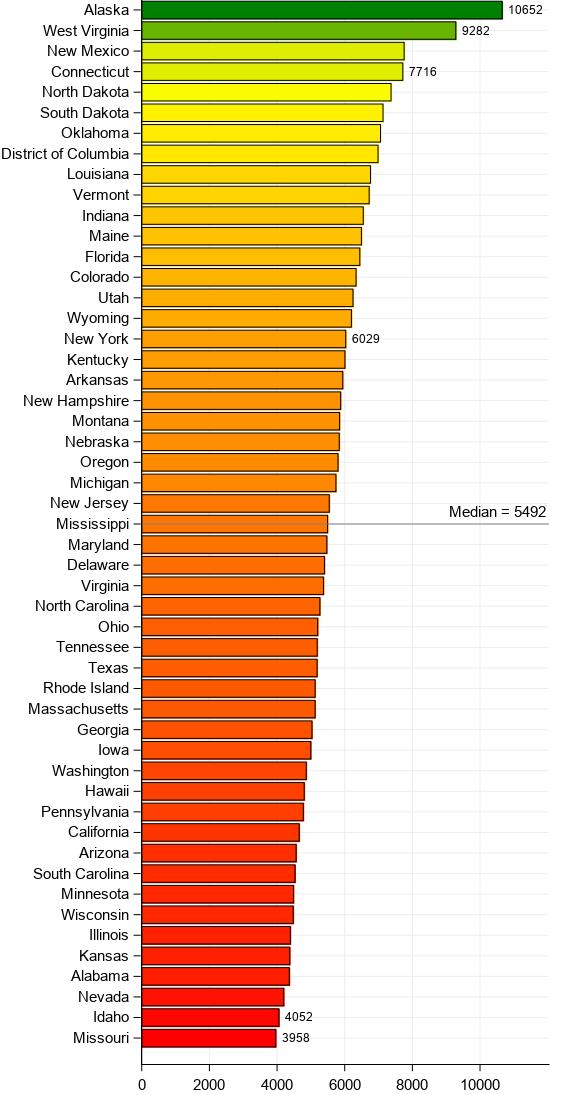
There are two dimensions that need to be explored further: HIE availability, and HIE use. We are concerned here primarily with use and recognize that it is only half the problem. Our simple observation is that the two states with best immunization penetration as of this writing, and the two states with the lowest, are not engaging their HIEs to identify, promote, record, and track immunization. Alaska’s COVID-19 vaccination plan does not mention any use of its fairly robust HIE system. Similarly, West Virginia does not plan to use its HIE platform to streamline its COVID-19 vaccination efforts. Interestingly, the vaccination rates are much higher in Connecticut than New York, which has one of the nation’s best HIE systems while Connecticut is still struggling with its HIE. At the other end of the spectrum, Missouri does not elaborate on how specifically it intends to use its several HIE platforms, neither does Idaho’s plan envision any role for its HIE in the vaccine rollouts.
We propose five ways that HIEs could accelerate mass inoculation for optimal public health impact.
Simplify identification and prioritization of high-risk individuals
After healthcare and essential workers, the elderly and those with specific medical conditions are next in line to receive the vaccine. Public health officials could use HIE data to easily assemble a roster of age-eligible individuals, and those with vulnerable conditions, reach out to them, and ensure that they are inoculated.
Facilitate monitoring of vaccination campaigns
Once a list of priority individuals is prepared, public health officials can—via the HIE—monitor their vaccination status in real-time. Because inoculation is distributed at a given date, time, and location, the HIE is a natural, accessible, reliable, and convenient way to collect and merge the vaccination records onto a single dashboard.
Expedite monitoring and reporting of any potential side-effects
The side effects of the vaccine, if any, could be identified and reported via an HIE. In addition to providing direct real-time medical benefits during an encounter, over time and in aggregate, these platforms enable health officials to assure the public about the safety of the vaccine. At the very least, HIE platforms can be a crucial source of information if there are reactions. Without such a system, investigations of any reported side effects and root-cause analysis will be immensely time consuming. Such delays would create a vacuum in which misinformation and conspiracy theories would flourish and erode public’s trust in the vaccines, leading to horribly detrimental results.
Help with management of overburdened medical facilities
Because HIEs have a longitudinal view of a patient’s medical records, officials and researchers can easily determine if an individual is vaccinated or could have developed natural immunization due to prior infections. They will also be able to quickly determine when—on a population basis—a region is likely to have herd immunity.
Further, HIEs can make it very easy for medical providers to know a patient’s prior status to each encounter and can organize their panels accordingly. Hospitals could use this information to better manage their facilities and strained resources; knowing if an individual poses infection risks would allow facilities to prioritize care provision, determine the need for additional COVID-19 testing, and decide who they must treat in isolated wards.
Help with integrated delivery networks like Veterans Affairs to reach their patients
Most HIEs are provider-to-provider networks, and typically do not have the ability to “reach out” to patients or even provide them access to their own information. An important exception—and great example—of how an HIE opens the aperture of patient engagement happens every day at Veterans Affairs (VA) facilities, which stay connected to patients and beneficiaries through their Blue Button services. VA runs the largest electronic medical record system in the United States; it could easily and proactively contact veterans who receive health services inside and outside VA, suggest places where they can be inoculated, and keep track of this special cohort all in one place. VA would serve as an example of best practices of how to roll out and monitor Covid-19 distribution.
In short, state- and enterprise-wide HIEs could help officials identify, prioritize, contact, and keep track of individuals who receive the vaccine. Indeed, without leveraging our tremendous investment in HIE platforms, the current road to recovery will be longer, slower, and much less effective.





Commentary
Five ways that health information exchange can help with vaccination efforts
February 1, 2021