The following is an excerpt from Reopening America: How to Save Lives and Livelihoods, a report published May 28, 2020 where Brookings experts offer ideas to help policymakers protect lives and save livelihoods in the midst of the current COVID-19 pandemic.
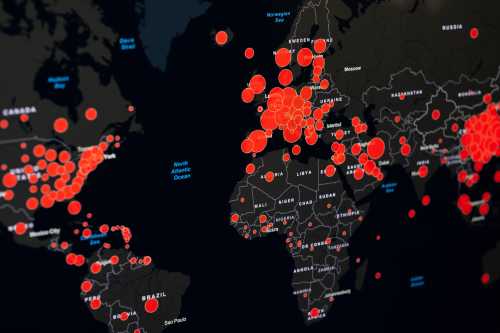
 The COVID-19 pandemic has killed over 300,000 people worldwide to date and has led to large reductions in economic activity as people take steps to protect themselves and as governments implement policies designed to control the virus’ spread. In the United States, these intense public and private social distancing efforts have indeed helped to control spread of infection, but have come with mounting economic costs and potential health risks of their own. Across the country, state and local governments are grappling with decisions about when and how to reopen workplaces, schools, and social venues and how to create an environment in which their citizens feel safe enough to resume these activities.
The COVID-19 pandemic has killed over 300,000 people worldwide to date and has led to large reductions in economic activity as people take steps to protect themselves and as governments implement policies designed to control the virus’ spread. In the United States, these intense public and private social distancing efforts have indeed helped to control spread of infection, but have come with mounting economic costs and potential health risks of their own. Across the country, state and local governments are grappling with decisions about when and how to reopen workplaces, schools, and social venues and how to create an environment in which their citizens feel safe enough to resume these activities.
Decision-makers must balance the imperatives for reopening to restore economic activity, education, and social life against the epidemiological risks of renewed transmission. Reopening too soon, or without the right epidemic control measures in place, is likely to produce additional waves of infection. Experience from other epidemics suggests these waves could produce surges of infection as high or worse than what the country has experienced so far. The science of epidemics tells us clearly that until a large fraction of the U.S. population has immunity—whether via a widespread vaccine or recovery from previous infection—the risk of resurgent infection will not go away. Given that a successful vaccination effort is likely many months into the future, and that we are currently far from widespread immunity, can the risks of reopening be mitigated or managed? Is there a “middle path” between indefinite shutdown and a freely spreading virus with inevitable high tolls of disease? In this essay, I argue that testing and modeling can help us navigate the uncertain terrain ahead.
INVESTING IN TESTING
The answer may lie in testing, as investment in a strong capacity to test Americans (for presence of or immunity to COVID-19) and policies based on testing have the potential to substantially mitigate the spread of infection, facilitating reopening some or all of the shuttered parts of American life while managing risks. Testing could be used in at least three different ways. First, testing to detect active infections could be combined with contact tracing (identifying those who may have been exposed) and quarantine to help contain emerging clusters of disease. Given sufficient test-and-trace capacity, this type of policy could replace some or even potentially all of the mass social distancing measures currently being used to contain epidemic spread. Other countries (including New Zealand, South Korea, Singapore, and Germany) are using versions of this approach already.
Second, even in the absence of contact tracing, sufficiently widespread and accurate testing could be used to adjust social distancing adaptively— turning shutdown measures on or off to respond to resurgent epidemics, exempting those who might be immune from distancing, or emphasizing protective measures for those at highest risk. Some states in the U.S. are already working toward this goal.
Decision-makers must balance the imperatives for reopening to restore economic activity, education, and social life against the epidemiological risks of renewed transmission. Reopening too soon, or without the right epidemic control measures in place, is likely to produce additional waves of infection.
Third, testing can give scientists much more accurate (and much needed) data to inform our understanding of who is at highest risk from COVID-19, how much spread is occurring among people with no symptoms (especially in children), and how much immunity the U.S. population is developing. These data can, in turn, lead to better projections and better planning.
THE CHALLENGE OF TESTING
Testing comes with its own challenges, as to be successful in mitigating an epidemic, any policy involving testing must be carefully crafted. Policymakers designing a testing approach must consider a number of factors. First, at least two different types of tests are available that give different information: whether a person is currently infected or whether a person has antibodies indicating they have had the disease in the past. For either kind of test, a testing regime must consider how many tests can be administered per day, how accurate the tests are, and how quickly the results become available.
In addition, a policy must define who is given the test—for example, to anyone with symptoms, to those employed in essential parts of the economy, to a random sample of the population, or to highrisk groups.
Finally, a policy must define specific containment actions and how the information from the tests will be used as part of these. Actions that may be part of such a policy include quarantining those with active infections, tracing the contacts of those who are sick, releasing those with immunity from workplace closure precautions, and so on. Many of these come with their own considerations such as how much capacity is there to trace contacts quickly, and what fraction of people will adhere to social distancing or quarantine rules.
The success of any particular configuration of testing-based policy in containing disease outbreaks will depend in part on the choices above (features of the policy) and in part on factors outside policymakers’ control (features of how the disease spreads). These factors include what fraction of cases of COVID-19 are asymptomatic, how contagious those with active infections are and for how long, and the length and degree of any protection conferred by antibodies.
THE VALUE OF MODELING
Given the complexity of these choices, and the uncertainty about many of the factors above, decision-makers considering a testing-based policy will benefit from the use of modeling. Quantitative dynamic models have been used effectively as policy tools in many previous epidemics, both to forecast the potential course of spread and as “policy laboratory” to understand the potential consequences of interventions. When confronting such a complex challenge, this type of model offers important advantages for policy design over reliance on either “mental models” (intuition) or the use of data alone. They allow counterfactuals and projections across diverse settings to be considered, past experience and extensive theory from combatting past epidemics to be incorporated, and experiments with many different policy options to be conducted within the model in ways that would not be feasible or ethical in the real world. For some types of model, the kind of diversity (demographic, geographic, social, and medical) that characterizes countries such as the U.S. can be taken into account to yield insights that are not “one size fits all.”
The use of models is not without drawbacks, and it is essential that modeling be used effectively and responsibly, following best practices on the part of both model designers and model consumers. But such models offer enormous potential to help answer key questions in the current situation, such as: How much testing and tracing capacity would it take to relax some or all social distancing without creating a large second wave of infection? What is the best way to use testing across a wide range of scenarios and uncertainty? Quantitatively, how well might various testing policies do—how many new cases would still occur, how quickly, and for whom? Models can also help tune policies to be as efficient as possible—maximizing the degree to which key economic and educational activities can be resumed while minimizing epidemiological risks. An example of the insights that such models can offer for COVID-19 containment policies based on testing can be found in the TRACE project, which evaluates thousands of potential policy configurations to find options that are robust across the enormous uncertainty facing decision-makers.
In the search for a “middle path” forward—a path that avoids the harms to health and the economy of either indefinite lockdown or unmitigated spread of the virus until widespread immunity offers a more lasting solution—testing can play a starring role, and models can help policymakers design approaches that are as effective, as efficient, and as robust to uncertainty as possible.
The Brookings Institution is committed to quality, independence, and impact.
We are supported by a diverse array of funders. In line with our values and policies, each Brookings publication represents the sole views of its author(s).





Commentary
Reopening America: The value of testing and modeling
July 2, 2020