Slowly, but hopefully surely, the U.S. is providing more of its citizens with the security and advantages of health care. Following the passing of the Affordable Care Act, millions more Americans are being covered by insurance. While many question marks remain over the future of health care reform (many of which have been covered on this blog), the general direction is clear. More people than ever are covered and some of the early missteps have been corrected. But we need to focus on health and well-being, not just health care and move policy in that direction.
The Colorado story
The latest success story comes from the state of Colorado, where the proportion of residents without health insurance has dropped to a record low of 7%, down from 14% pre-ACA, in 2013 – and from a peak of 16% in 2011, according to the official Colorado Health Access Survey released today.
Almost half a million extra Coloradans were added to the Medicaid rolls between 2013 and 2015, Just 2.5% of Coloradan children (those under 19) are now without insurance, down from 7% percent:
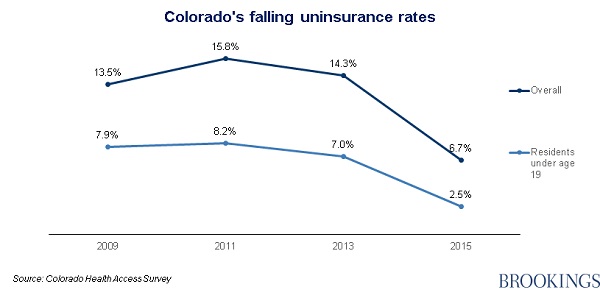
As expected, most of the gains have come at the bottom of the income distribution: and the uninsured rate for those earning at or below 300 percent of the federal poverty level (FPL) fell to 8 percent from 21 percent.
Not all the news is good, of course. There has been a slight uptick in the number of Colorado residents complaining that they were unable to get a medical appointment when they wanted: a sign that supply is struggling a little to keep up with demand. Hispanics continue to hold last place for coverage, with 12% still not covered (though that figure is nonetheless sharply down from 22% in 2013). But in the round, the last few years for Colorado health care have been ones of great achievement.
Now what? Focus on the Social Determinants of Health
But nobody should rest on their laurels. There remain challenges of coverage. But it is also time to start looking to the next stage of health reform: beyond simple coverage towards the active promotion of health, wellbeing and opportunity.
Two decades ago, a set of bipartisan, radical welfare reforms shifted the focus of provision for working age adults and their families towards promoting work and independence. ‘A hand up, not a hand out’ was the slogan. While arguments continue to rage over the effects of the reform, few can doubt that they changed both the substance and symbolism of American welfare provision. The motivation was to shift from safety net to springboard; and as one piece of evidence for success, employment rates of single parents jumped dramatically in the wake of reform (assisted by a strong economy and a more generous Earned Income Tax Credit). The assumption had been that welfare recipients couldn’t or wouldn’t work. That assumption was wrong.
The next wave of health reform could follow a similar pattern. With a system in place that ensures basic coverage, the next goal should be to shift to a model of partnership rather than paternalism. Spending should shift towards prevention rather than expensive treatments. Individuals ought to be incentivized to invest in their own health and wellbeing. Funding can begin to be configured around goals of broad wellbeing, rather than simply the narrow provision of care: better family planning and improving maternal education, for example, can have a powerful impact on child health outcomes. Home visiting programs can reduce the need for medical care while providing infants a better start in life. Early childhood education instills better nutrition and good health habits at a young age. Current evidence suggests that some reallocation of resources in this direction will both improve health and save money at the same time.
None of this will be quick or easy. Nor should planning for the next stage dampen celebrations of the progress made in recent years. But in the long run, the reforming vision must be not be limited to a universal health care system but the building of a universal health system. To improve opportunity individuals need not just health care but new and more effective programs and a willingness to do their part in taking advantage of whatever is on offer.
The Brookings Institution is committed to quality, independence, and impact.
We are supported by a diverse array of funders. In line with our values and policies, each Brookings publication represents the sole views of its author(s).




Commentary
From health care to health – the next agenda
September 1, 2015