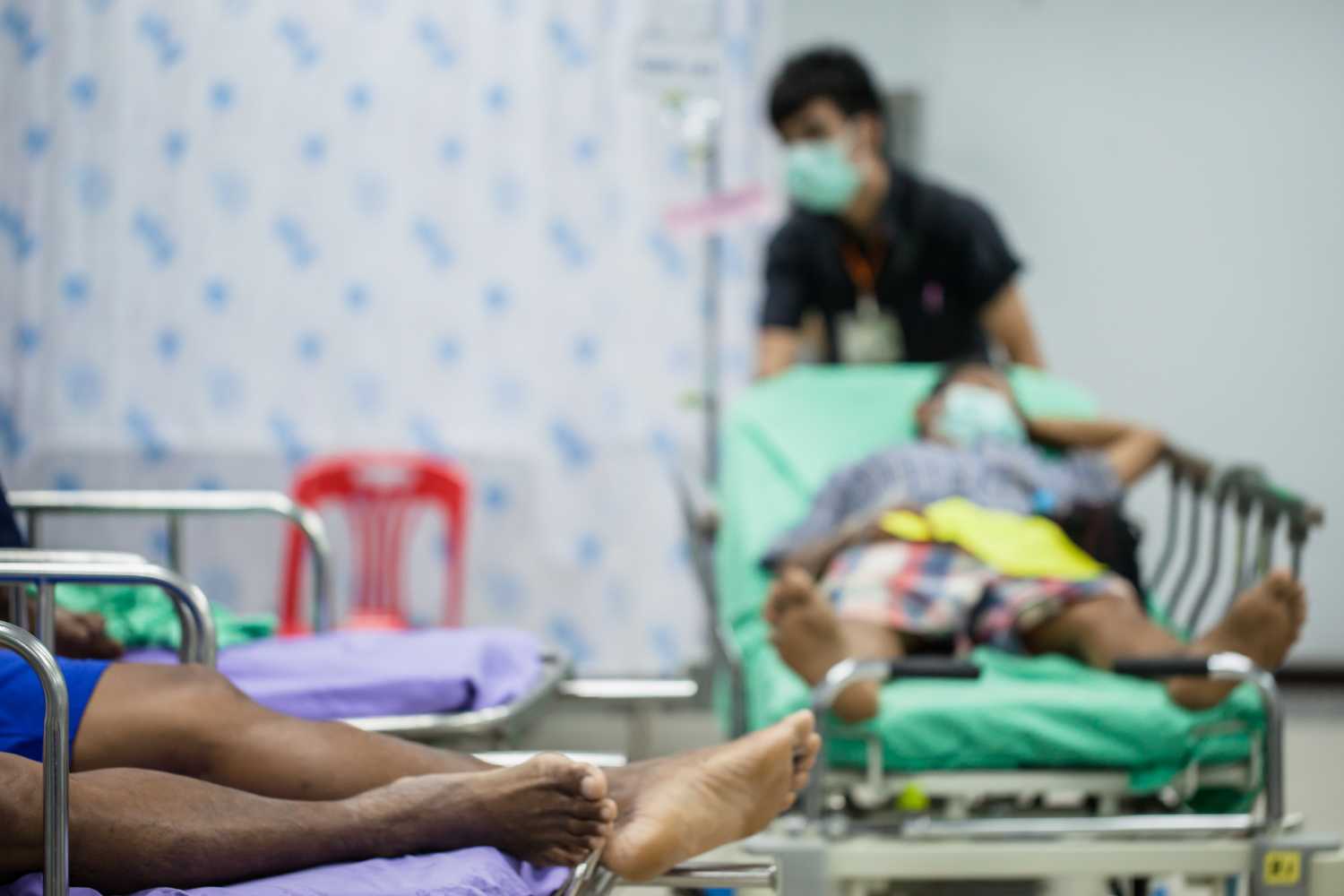
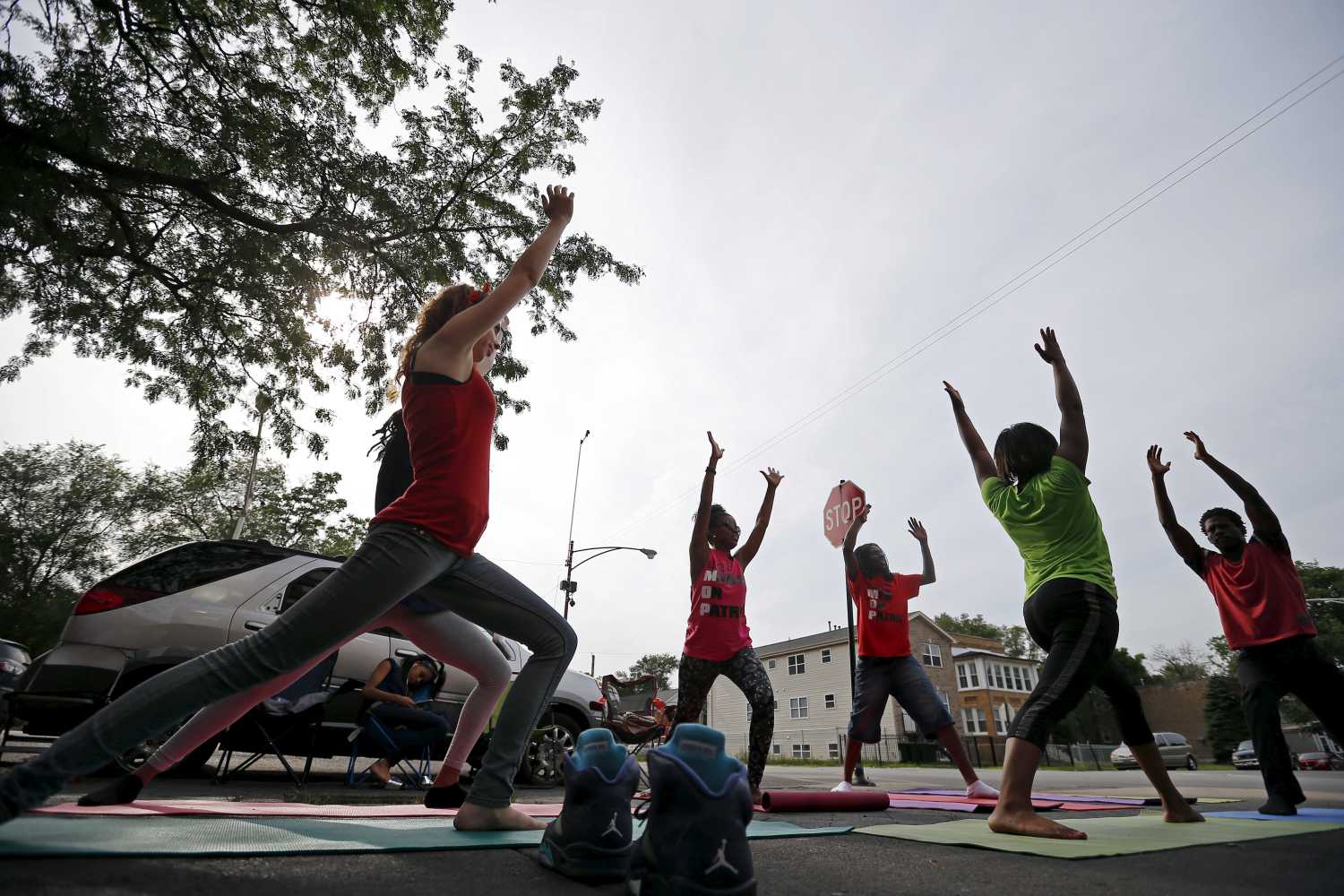This brief is part of the Brookings Blueprints for American Renewal & Prosperity project.
The American health system is rife with gaps and inequities. The result is inadequate or no insurance and services for millions of families and unacceptable differences in resources and health conditions related to income, race, and location. Resources are misallocated, the health care infrastructure in many communities is inadequate, and our financial support for health coverage is disjointed and inefficient.
It is time to move towards a health system in America that provides adequate, affordable, and accessible care to all U.S. residents, and that reaches this goal by refining existing programs, correcting the subsidy system, and using the power of federalism. Achieving this goal requires us to:
- Create an effective, grassroots community health system by expanding health clinics, creating other local points of access, focusing on social determinants of health, and addressing gaps in Medicaid.
- Reform the tax treatment of employment-based coverage to create universal subsidies that allow effective choices of coverage in an arrangement that could be described as “Medicare Advantage for All.”
- Use program flexibility and state innovation to create a truly national system with appropriate state variation.
Challenge
The COVID-19 pandemic has laid bare the profound weaknesses of the American health care system, in particular the enormous inequities that pervade it. The virus has highlighted these gaps and made them worse. It has underscored the fact that decades of widespread dependence on employment-based coverage – a byproduct of the tax treatment of health spending – means that Americans must change or lose their coverage if they change or lose their jobs. Layoffs during the pandemic meant that as many as 7.7 million workers and 6.9 million dependents lost health coverage as well as a paycheck and have had to scramble to try to find alternative affordable insurance. The pandemic has also exacerbated the sharp differences in health services and outcomes between racial and income groups that have long existed in the system. And it has shown the weakness of our public health system, overwhelming already overstrained and underfunded local clinics and health workers.
Redesigning this system will be no easy task. Health care is a polarizing issue, and in this enormous country there are big differences in attitudes and approaches to health coverage. But COVID-19 has focused attention on the need to address the gaps while preserving popular features of the current system. Accomplishing that will not be easy, but there is a pathway that combines liberal and conservative principles and so could attract White House and bipartisan congressional support.
Limits of historic and existing policies
While the United States can claim to provide among the world’s highest quality health care, the country has struggled for decades to create a health system for all its residents. Most other developed countries have established systems that enshrine broad national principles of universal coverage and are relatively consistent in ensuring at least basic care throughout the nation. The American “system,” however, is a collection of mini-systems, each based on different eligibility criteria, different budgeting frameworks, and different financial obligations by patients. We have a federal-state system for the poor which varies across the country (Medicaid). There is a national social insurance program for older people (Medicare). We have yet another system for some working people (tax advantaged employer-sponsored coverage). Meanwhile, millions of other working people obtain services through another system (state-level exchange plans). And still millions of households fall between eligibility criteria for these programs or cannot afford coverage, and so they remain uninsured.
The inequities and gaps in this system are a national disgrace. One result is significant differences in the medical resources and outcomes associated with different population groups. For instance, Hispanics and Black Americans have significantly worse health than whites in America. Local conditions as well as inadequate health resources exacerbate these differences; people raised in medically under-resourced and minority areas tend to experience poorer health throughout their lives when compared with others. Community conditions, including schools and other local services, transportation, and air quality, are an important factor in this pattern.
Another feature is inequities and gaps associated with employment. Only 89 percent of workers are employed in firms that offer health insurance. For them, the full value of their compensation in the form of employer-sponsored insurance (ESI) – with the employer share valued at an average of nearly $16,000 in 2020 for family coverage – is free of federal, state, and payroll taxes (known as a “tax exclusion”). But this tax break is much more valuable to highly paid workers than to low-paid employees who pay little or no federal income tax. Moreover, even this regressive tax break is unavailable to part-time workers or others who cannot afford to purchase family coverage offered by the employer.
The availability of ESI and the regressive tax subsidy varies widely by size and type of employer. Virtually all large firms offer tax-subsidized coverage. Meanwhile, for small (3-199 employee) firms, and in the retail, agriculture, and service sectors – where there is a higher proportion of minority and lower-paid employees – only about half offer insurance to their employees.
It is true that workers without the offer of ESI may be eligible for progressive, income-related federal subsidies for exchange plans created by the Affordable Care Act (ACA), but only if their incomes are between 100 percent and 400 percent of the poverty rate (i.e. between $12,760 and $51,040 for an individual in 2021). The ACA sought to help by requiring all states to make Medicaid available to more families, but the U.S. Supreme Court struck down that provision and several states declined federal funds to expand Medicaid coverage, leaving many of their residents without any affordable coverage.
Thus, while landmark pieces of legislation—including those that created Medicare and Medicaid in the 1960s and the ACA—have provided good health coverage to millions of Americans, it has been in a piecemeal way and unacceptable gaps and inequities remain. It is time for decisive and consistent action to address this situation.
Policy recommendations
Strategic principles for action. There are five broad principles of design and approach that would achieve a more equitable and effective system and likely would command broad support in the country. They should undergird a bold plan to strengthen our health system.
- The system should guarantee adequate, affordable, and accessible care to all U.S. residents. While there are significant differences of opinion on exactly what services should be available to everyone and how a system should be organized, the idea of at least basic services that are realistically available and affordable to all is broadly accepted in America.
- There must be a strong community health system with an emphasis on social determinants of health. We have learned that for effective and equitable health care to be made available, especially in lower-income and minority neighborhoods, there must be robust local health institutions backed by Medicaid and other coverage sources. Attention must also be paid to the non-medical factors that influence health, such as housing and transportation.
- States must be allowed to adapt and innovate within national goals and a national framework. State-level experimentation—within agreed national boundaries—is essential for the system to adapt and improve over time. By receiving waivers from federal rules, states have over the years done much to expand care and explore better health delivery systems.
- There needs to be horizontal equity in financial assistance. The degree of tax relief or direct assistance for working-age households to pay for insurance or care varies widely depending on employment and other factors; it needs to be consistent. Similarly situated households should receive similar financial help, wherever they reside and wherever they work.
- It is better to build on or adapt existing programs and institutions than attempt radical change. Most Americans are generally skeptical about large changes in the health care delivery system, even when the result is likely to be an improvement. Fortunately, there are ways to modify existing structures and programs to move towards greater effectiveness and equity.
Building on these strategic principles, we must commit to addressing the inequities and shortcomings of the current system by building on its strengths and modifying key features in line with the strategic principles. That suggests an approach with three key elements: first, creating an effective grassroots population health system; second, achieving equitable subsidies for insurance by moving from employer-sponsored insurance to “Medicare Advantage for All;” and third, creating a national system that encourages a degree of state variation.
Create an effective grassroots population health system
An equitable and effective health system requires attention both to the availability of medical resources and a stronger focus on community-based strategies to address “upstream” social factors that are linked to health.
Action: Expand community health centers. The first step should be to expand the system of community health centers in underserved areas and provide greater long-term funding certainty. These clinics serve roughly one out of every 12 U.S. residents. With direct support from the federal government, local support, and Medicaid and Medicare funding, the clinics provide a broad range of primary care services to families, including uninsured and undocumented patients. Providing free care to some families often strains the business model of clinics; those that offer good service to the uninsured tend to attract more patients who are unable to pay, which can jeopardize their finances—a classic case of “no good deed goes unpunished.” Many health centers also partner with other community institutions to tackle social determinants, such as housing needs and social services.
The clinic system is the core provider of primary care in most low-income and underinsured communities. Moreover, the system has attracted bipartisan support for many years. Thus, building on it could attract broad political support.
As a key tool to address inequities, federal funding for such Federally Qualified Health Centers (FQHCs) needs to be expanded, with an emphasis on areas with greatest need.1 While direct federal funding for community health centers has been affected in 2020 by COVID-19 spending and uncertainties in the congressional budgeting process, in recent years it has averaged just under $6 billion (clinics also receive payments for services to patients through Medicaid, Medicare etc.). That commitment needs to increase for centers to play their full role as the primary care system for millions of U.S. residents. In addition, federal, state, and local agencies should take a variety of steps to enable different programs and private entities to coordinate funds to enable FQHCs to become hubs for both medical services and for addressing the social determinants affecting their patients’ health. Local nonprofit hospitals could also provide more help in this funding task if there were clearer federal guidance for using community benefit funds to support clinics.
Action: Make additional access points available. In addition to the system of community health centers, we need to encourage the creation and expansion of other health hubs and health access points in underserved areas that would be more convenient to families. This includes financing school-based clinics to provide a broader range of services to children and to their parents as well as housing-health partnerships.
The federal and state governments can foster the creation of more access points in several ways. It can expand the federal Accountable Communities for Health initiative, which helps communities deliver health services in a variety of settings and in combination with other needed services. It can also remove uncertainty about federal regulation. For instance, there is often local hesitation to be creative in siting health facilities in housing projects, community centers, and other locations, out of sometimes misplaced concerns about privacy laws, legal liability, and other practical issues. The federal government, along with states, could help calm these concerns by providing greater clarity on the rules and by issuing “safe harbor” guidance on the best approaches. Helpful, too, would be state and local programs to encourage primary care workers to come to high needs communities, such as Maryland’s Health Enterprise Zone program.
Many of these approaches would be enhanced by greater use of community health workers and organizations that help link families more effectively with the health system. Both government and private sources are needed to build out this important part of the health system infrastructure. Better linkages and communication would also be enhanced by making permanent some of the COVID-19 emergency payment and flexibility granted for the use of telehealth services, which make access to health providers easier for many families.
Action: Focus on social determinants. Another necessary step is to create a better balance between spending on medical services—clinical health interventions—and on non-medical services targeting social determinants, especially within communities exhibiting poorer health. We have learned that an individual’s health is significantly influenced by neighborhood conditions, such as the quality of housing, the availability of transportation, childhood and adult stress levels, nutritious food, and other non-clinical factors. In all neighborhoods and families, these factors influence health outcomes and contribute to chronic conditions, and so in under-resourced areas, including poorer neighborhoods and in many Black, Latino and Native American communities, the deleterious impact on health is greatest. Thus, addressing these health influencers will be disproportionately beneficial for many communities with poor health status.
Focusing on social determinants does require more research for policy and budgeting to be efficient. While there has been a sharp increase in research in recent years, it is still often very difficult to determine with confidence the exact relationship between investing in different policy approaches and the degree of health improvement. Government and philanthropy need to support stepped-up research in this area.
It will also be necessary to make changes in department budgets and to explore budgeting tools to allow funds to be used more flexibly through a variety of techniques. Special bodies, like the U.S. Interagency Council on the Homeless or state-level Children’s Cabinets, coordinate cross-department spending and are models for addressing social determinants. Waivers from federal rules are also a valuable tool (see below). Currently the U.S. is an outlier among developed countries in the ratio of spending on medical care—especially hospital and outpatient procedures—compared with social services. To improve the health status of minorities and others who are more likely to live in under-resourced communities, government at all levels must make it easier for health programs to devote more of their resources to housing, nutrition, transportation, and other health-related non-clinical services. Jurisdictions can build on such examples as Congress and the Trump Administration giving Medicare Advantage plans more flexibility to provide non-clinical services and using Medicaid waivers to enable states to combine medical and other services for certain populations.
Action: Create an option for non-expansion states. The federal-state Medicaid program is the crucial financing and health services foundation of the health system for lower-income households, and so a necessary step to advance equity and quality is to enhance Medicaid’s effectiveness. One way to do this is for states to introduce more comprehensive managed care, which allows more integration of medical and other services to improve enrollee health. But even more urgent is the task of addressing the gap in available services to many lower-income families within so-called “non-expansion states.” This gap arose when, in 2012, the U.S. Supreme Court ruled that the federal government could not require a state to accept federal funds to expand Medicaid eligibility for many low-income adults previously not qualified for coverage in that state. More than a dozen states declined to do so and 12 have still not agreed to the expansion. The ACA exchange plan subsidy structure was based on all states expanding Medicaid.
For the states that still resist Medicaid expansion, a solution could be to provide these states with the federal funds foregone by not expanding Medicaid in order to enroll low-income households in ACA exchange plans or to allow these states to create their own programs that could achieve the same goals and coverage as the ACA’s Medicaid expansion. States that have already expanded Medicaid would not be given this opportunity. It could be challenging to do that while maintaining the incentive for expansion states to continue their enhanced Medicaid programs, but experts with different political philosophies have suggested ways that challenge might be overcome.
Achieve equitable subsidies for insurance: Transition from employer-sponsored insurance to Medicare Advantage for All?
In addition to better access for underserved communities, an equitable and effective health system also has horizontal financial equity—in other words, functionally equivalent assistance for all to help afford adequate insurance and care regardless of employment and geography.
Action: Replace the tax exclusion with universal tax credits. Over the last 30 years, a variety of proposals have been offered by Republicans and Democrats to create a system of subsidies that is more consistent across income levels, irrespective of type of employment and more progressive in relationship to income. The ACA’s exchange plan subsidies, expanded Medicaid, and the special so-called “Cadillac” tax on generous ESI plans—twice delayed and then repealed by Congress—all moved in that direction.
A subsidy system that achieves a horizontally equitable, dependable, and progressive system of support for families to afford health coverage and costs could be achieved by gradually replacing the ESI tax exclusion and ACA exchange credits with a universal system of income-adjusted, refundable, advanceable, federal tax credits.2 Many Republican lawmakers, as well as Democrats, over the years have been attracted to progressive tax credits for insurance. Currently, the individual tax exclusion for ESI involves over $270 billion in annual foregone federal tax revenue. This enormous and regressive tax break could be gradually transformed into a system of progressive credits that would leave most middle-class workers little affected but provide more financial help to lower-paid workers. Such credits could be used for the cost of health insurance plans that meet federal standards (including insurance combined with Health Savings Accounts), as well as plans offered through ACA exchanges. Ideally the refundable credits would begin to kick in at the level of income where eligibility for Medicaid ceases; indeed, a version of the refundable credit system could be part of an alternative to Medicaid expansion in non-expansion states. A more modest, transitional proposal, advanced by President-elect Joe Biden and others, would be to eliminate the “firewall” around ACA exchange subsidies (which denies exchange subsidies to households that are eligible for affordable ESI) and allow households with an offer of ESI to instead enroll in subsidized exchange plans.
With this equitable subsidy system in place, all working families would receive similar assistance, linked to need, to afford adequate health coverage without regard to their place or sector of employment, size of employer, and whether they worked part-time or seasonally. Coverage could be obtained through ACA exchanges or from another source meeting federal insurance standards. The principal gainers from this subsidy system would be lower-paid employees, minorities, people sporadically in the workforce, and those often changing jobs—precisely those households who today experience the highest levels of uninsurance.
Under this reform, the health insurance role of most employers would not end, but it would change. Generally, employers would retain their bookkeeping function of making plans available and handling payroll deductions to facilitate payments to plans, as well as making withholding adjustments in paychecks to reflect an employee’s eligible credits. Employers could continue to sponsor insurance—that is, pay for it as part of compensation; in this case the value would be added to the employee’s taxable compensation but also would be eligible for the employee’s refundable tax credit.
This subsidy reform would substantially eliminate the structural inequity associated with employment-based coverage. Working families would be able to get the same choices of insurance and the same financial assistance whether they worked for a large firm, a small firm, were self-employed, worked part-time, or were temporarily unemployed, and whether they worked in the service sector, agriculture, or a Fortune 500 company.
Action: Move to Medicare Advantage for All. Structuring a subsidy system in this way would not only help achieve horizontal equity. It could also help the country edge towards a health system in which the form of coverage ultimately is similar for the vast majority of U.S. residents, whatever their income, work status, or age. This would be a system with choice among managed health care plans in which enrollees receive federal (and for some, state) subsidies to help pay for premiums, and with plans also receiving risk-adjusted capitated payments to reflect the insurance risk of enrollees with different health histories. Medicare Advantage plans already have a structure like this. And with about 90 percent of Medicaid beneficiaries in managed care plans and about two-thirds of workers with ESI enrolled in some form of managed care or network coverage similar to Medicare Advantage plans, the future structure of coverage would evolve into something that might best be described as “Medicare Advantage for All.” By incorporating key features of existing programs and plans in this way, the proposed reform would be a gradual change in the coverage systems Americans are familiar with, not a radical departure.
Create a national system with state variation
A national system of health care does not have to look the same everywhere. What it must do is conform everywhere to national goals and values: adequate, affordable, accessible care for all.
A degree of variation is both necessary and desirable, and America’s system of federalism can enable our health system to build consensus and to evolve. In contentious areas of policy, federalism can allow ideas to be introduced in some states and observed by others, paving the way for broader acceptance. The western states, for instance, created the momentum for women’s suffrage, and state action and experience helped break down opposition to same-sex marriage. Similarly in health care, concerns and skepticism about approaches to health system design, from reinsurance pools to questions about the effectiveness of some social determinants of health, can be field-tested first at the state level rather than facing an “all or nothing” political test at the national level. The earlier example of states being permitted to expand Medicaid or introduce a variant to achieve the same objective is another example of using federalism to ease the pathway to reform. Allowing states to explore alternative ways of reaching the same goal and then comparing the results increases the likelihood of future consensus.
Action: Make greater use of waivers. The waiver authority granted by Congress in Medicaid (Section 1115 waivers) and the ACA (Section 1332), together with other program waivers, are important federalism tools that allow states to request temporary variations in the operation of these programs so they can explore alternative ways to achieve program objectives. Waivers have been used extensively in Medicaid, with states often adopting other states’ approaches, and have been the driver of broad changes in the program over time. The more recent ACA waiver authority also led to several state requests under the Trump Administration, although Congress needs to clarify that states can integrate different health programs under 1332 waivers. Existing waiver authority should be used more extensively by the Biden Administration, and Congress should enact more waiver authority in housing, social services, and other programs to allow more cross-sector initiatives that seek to improve health outcomes.
While waivers, and federalism in general, constitute a powerful and beneficial tool to adapt and innovate, there does need to be appropriate safeguards to assure that the goals of a more equitable and efficient health system are achieved everywhere. Waiver authority is set in statute, but the extent of that authority is largely interpreted by the administration in power, and some analysts argue that certain waiver requests have exceeded the statutory authority. Moreover, the granting of waiver requests typically reflects the philosophy and goals of the White House rather than a “let a thousand flowers bloom” vision of state-led innovative federalism. That shortcoming of waiver authority could be addressed by widening the waiver process to permit alternative waiver application routes, including waivers recommended by a commission representing states, Congress, and the administration.
Conclusion
A byproduct of the COVID-19 pandemic is a better understanding today of the structural weaknesses of the U.S. health system and a growing appreciation and acceptance of what a reformed system should look like. Still, Americans hesitate to embrace big change in health care, even when they agree on the need for it. Fortunately, reform does not require a wholesale abandonment of the current system and the implacable opposition that likely would be triggered if that were attempted. There are many programs and elements of the current system we can build on and make consistent. Moreover, many of the key ideas discussed in this report have their roots in both political parties, and so, with genuine outreach to leading lawmakers on Capitol Hill, the Biden Administration could achieve bipartisan progress on health reform. Moreover, structural change does not have to come in the form of one giant bill; it can be achieved through a series of bills and administrative actions. Indeed, with a clear, shared vision of the objectives, some bold leadership, and a willingness to build on or remodel some existing parts of today’s system, there is a bipartisan path to an equitable, inclusive, and comprehensive American health system.
-
Footnotes
- Disclosure, the author is an unpaid board member of an FQHC system in the Washington, D.C. area.
- A refundable tax credit means that if a household’s calculated available tax credit exceeds its pre-credit tax liability, the household receives a government payment for the difference, The Earned Income Tax Credit is an example. And advanceable credit is one that can be integrated into paycheck withholding, so the recipient does not have to wait until tax filing to claim it.
The Brookings Institution is committed to quality, independence, and impact.
We are supported by a diverse array of funders. In line with our values and policies, each Brookings publication represents the sole views of its author(s).